Plantar-fasciitis (P.F.) is a seriously annoying, long lasting painful condition of the big ligament that passes along the sole of your foot – It will typically persist unless the repeated daily cycle of day time trauma and night time healing and the incessant aggravated damage through daily activity is interrupted.
Key Points:
Just a bit first about terminology – plantar-fasciitis (inflamed plantarfascia) – is rare, however Plantar-fasciopathy (aching in P.F.) – is extremely common. I’m going to stick myself out on a limb here (excuse the pun!) and say that PF is a painful symptom of other more complex issues. Classically, PF is caused by tightness/rigidity of the Achilles/plantar-fascia complex and is massively exacerbated by unstable or flat foot posture or activities involving lots of foot stress. This condition however rarely occurs in athletic individuals with loose, supple or well toned legs. Stretching legs and calf muscles is vital in aiding recovery.
When your PF has been torn and injured, your body repairs the injury with scar tissue. This forms as small pea sized lump (fibroma) that feels very tender and firmly attached. Repeated injuries = additional scar tissue = increased PF stiffness = increased vulnerability to further injury and foot compensation. Reducing and mobilising these fibromas is vital to aid recovery.
Heel spurs form on the base of your heel, created by the pulling action of your now (too) tight PF drawing bone in a little hook (spur) that feels pretty awful under your heels when walking bare-foot. Offloading this painful prominance underfoot is vital in aiding recovery.
Foot instability heightens the work and effort of your PF as it tries to keep you straight. A history of Flat feet means that your PF has to be worked harder to keep up. Supportive insoles can help offload the PF but typically they require to apply force to the foot in all the painful areas so be careful here! Orthotic insoles alone are not a long term solution but can be awesome as part of a treatment plan.
Wear soft bouncy shoes with good heel support. Modern sports style shoes like sketchers can help protect the PF by absorbing some of the jerky sharp forces that would otherwise hurt your poor foot! Avoid bare foot walking as much as poss, avoid tough hard heeled shoes, your feet love a bit of a change now and then so shake up the wardrobe 🙂
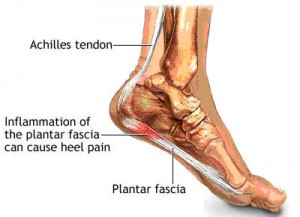
More information: The PF connects the bottom of your heel bone to the front of your foot (Below), your Achilles tendon attaches directly into the opposite surface of your heel bone and directly affects the state of the plantar-fascia- hence why I’ll keep going on about Achilles and calf tightness. The fascia of the sole of the foot continues in an unbroken sheath up your legs and hip and back finishing in the jaw. It provides an effective anchor for each muscle group to function but its main job is to connect the systems together.
Remember, PF is a symptom not a cause. It occurs due to a loss of other much bigger issues like balance, strength, hip & knee control hence why it can take years to fully develop and doesn’t miraculously self resolve. Hip strength is needed as strong hips stabilise your feet, this is why many people with flat feet have weak hips and vice versa.
Untreated this condition will rarely resolve itself within 9 months – Sometimes lasting for years. Steroid injections are useful if you are off for a walking holiday but won’t address the cause and therefore rarely reverse the symptoms. Typically PF will ebb and flow on and off for many years unless something significant changes.
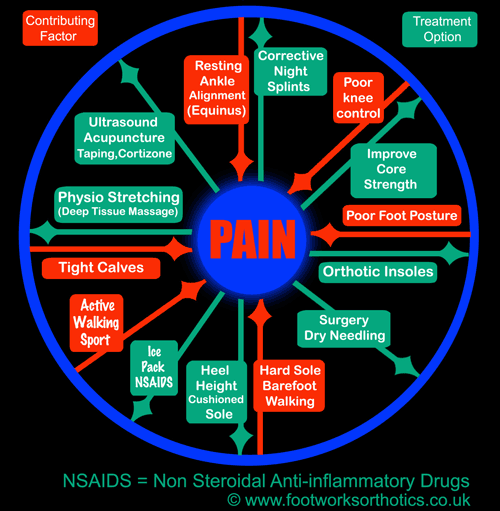
I have tried to list the main options for you to consider. Basically you need to do as many of these things as often and as regularly as possible – bear in mind that if you do nothing it’s not likely to go away by itself. (see below)
Orthotic Insoles
Wear supportive insoles as they aid the control of the movement of your feet through the day, protecting your feet from the excessive twisting and stretching movement on the insertion of the plantar-fascia at the heel bone. An incorporated slight heel raise from a good shoe also benefits by further reducing the tension of your calves. Prescribed Orthotic insoles differ enormously from simple off the shelf options in that custom orthotic devices can actively offload your PF to aid healing.
Stretching
Mobilise your legs, especially your calves and hamstrings every morning before walking and then stretch regularly through the day as your activity increases (to try to get some extra length in your calves and Achilles) – While we sleep our muscles and ligaments shorten and the foot is pulled into a relaxed posture with the toes pointing down – this period of rest allows the body to try to heal the injured area with scar tissue. Every morning a sudden increase in stess occurs when we force our feet into a 90 degree standing position as we haul ourselves out of bed. This can cause the newly formed scar tissue to tear/rip away causing extreme pain and yes you got it another injury to fix!. This pain typically lasts for only the first few steps and soon subsides as we continue to walk. However a short rest will bring on the pain again. Passive stretching prepares our muscles and the fascia for the activity ahead. Ask us for advice about dynamic stretching to maximise the effect of your stretches.
Strengthening
Work to improve your balance, especially on a single leg. If you are not sure what I mean – stand in front of a mirror and balance on one leg – Do you wobble? do your shoulders not stay straight? Your hip muscles support the alignment of your legs and pelvis but importantly also help to lift and stabilise your arch protecting your PF from too much load. Try to balance without wobbling for 30 sec on one leg.
How about standing on tip toes? Try it …. stand up as tall as you can be and hold for 15 sec – you will feel your tummy pull in, your buttocks engage and feel your calves and feet working hard.
Massage
This can be enormously effective as it addresses some of the other issues that are triggering the problem in your feet. Try a deep tissue sports massage twice a week initially to help reduce the stiffness and rigidity in your legs and feet. Tightness in muscles and the resulting reductions in ranges of movement in your joints transfers huge tension to the plantar-fascia compounding the problem. Unfortunately, a good massage will hurt a bit and you will find muscles you thought you never had. We look after our cars better than we look after our bodies – keep up a regular monthly massage to keep supple. Don’t forget to drink lots of water after any deep tissue or sports massage.
Mobilise your PF using a tough rubber ball on the floor or by using your hands. Part of the recovery of PF is achieved by reducing the size and rigidity of the fibromas that develop along your PF. In clinic we provide scar tissue reduction massage to help mobilise your PF, increasing the pliability and shock absorbency of your PF. Use a heat pack or hot water bottle to warm up and mobilise your PF before massaging it, after exercise or massage use Ice or cooling spray to help reduce the inflammation or bruising. Remember the application of Ice and heat can help control your body’s injury response and promote faster healing.
Shoes
Avoid very flat low heeled shoes and traditional flip-flops as the low heel forces the achilles and plantar-fascia to be put under increased tension. Also, avoid walking barefoot – always wear something cushioned around the house. Wear day shoes with a slightly more than average heel height to reduce the tension in your achilles. Avoid flat soled converse or thin soled daps or ballet shoes. Try fit – flops, HOKA, or sketcher shoes for improved cushioning at heel and smooth roll over the toes. Fortunately, there are many acceptably styled sport/dress cross-over shoes available, but you will have to spend hours searching online.
Acupuncture
This is another extremely beneficial treatment to release the tension affecting calf muscles and reduce inflammation in the plantarfascia. Effects can be accentuated through the use of electro-needling to increase the stimulation to affected or intended area. (Ben Tolson professional acupuncture)
Night time stretches
If you are really desperate and have exhausted all of the above …. There are a variety of devices that you can wear to keep your feet in a stretched position through the night. Unfortunately they generally look and feel like snowboarding boots and their bulk and rigidity are rarely appreciated by sleeping partners. (below left) These retain cheaply £30-50 but are pretty nasty to wear and impossible to walk with if you get up to go to the loo in the night.
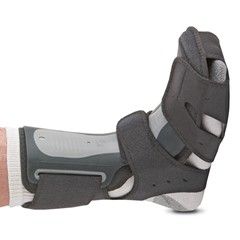

Footworks Orthotics clinic stock a vastly superior front fitting night splint (above right) which gives significant improvements to comfort. A well padded contoured aluminium shell works perfectly to maintain your foot in a stretched toes up position keeping tension on the plantar-fascia forcing it to heal with your foot in a functional position either when seated or whilst sleeping through the night.
Night splints are great because they give almost immediate relief to the sharp ‘getting moving pain’ that is characteristic of this condition.
Contact me directly if you think that this may benefit you.
Exercise
Don’t exercise hard unless you have properly warmed up and stretched really well before hand. Swimming is Ok as you swim with your toes pointing down, but take care stepping out of the pool – take time to sit on the side and do a few gentle mobilising stretches before walking. Cycling is great for fitness but you will find it causes your calves and hamstrings to tighten up – stretch after cycling!
Remember to stretch your legs and feet during and after exercise.
Other options:
Cortizone injection to reduce the acute inflammation (really painful injection but normally takes pain away for 3-4 months)
Rest
If you can afford to lie on your back and let the kids do all your work then your feet will heal beautifully in about 8 weeks and you will forget how horrendously painful this awful condition is!

I have had cortisone injections, and wear insoles but still suffer with pain on a daily basis. I do achillies streches but not religiously. Are there any good sites out there that sell fasionable sandals/shoes.
Same like Sian above I’ve been also having cortisone injections to help with the pain but it didn’t help to relieve the pain. Now I’m trying orthotics but it hurts like hell ;(
I’m wearing foot logics insoles for the past week, starting my day with exercises and trying to minimise long episodes of walking. I’m even doing stretches in bed before hobbling around (in slippers). I actually think this has come about as a result of the shocking back stiffness I have in the morning. It’s been a feature for years and I’ve just been letting it resolve as I get around in the morning, then exercise. Plus I’ve had a preference for totally flat shoes, without any arch support or cushioning and love walking. Now that I’m 59, this clearly isn’t going to work anymore.
It’s not as sore after walking in that 1 spot on the bottom/inside of the calcaneus which was getting consistently battered for a couple of months. There can be some twinges on the sides of the heel/ankle – and the other knee! I feel like I’m tending towards the outside of the affected foot and doing some awkward moves. But once I get going, can do a reasonably normal gait. Just can’t tell if it’s getting better. Thanks for the excellent advice & info. though.
I think orthotics are the best solution for reducing the pain, at least for me. Foot exercises can help a lot too, but it takes a lot more effort.
I suffer from all the above however I have only been wearing FitFlops! I had no pain when I started wearing then and now I have unbearable pain and constant pain! Seriously, FitFlops are not the answer! They cause foot fatigue and in my case they are the problem!